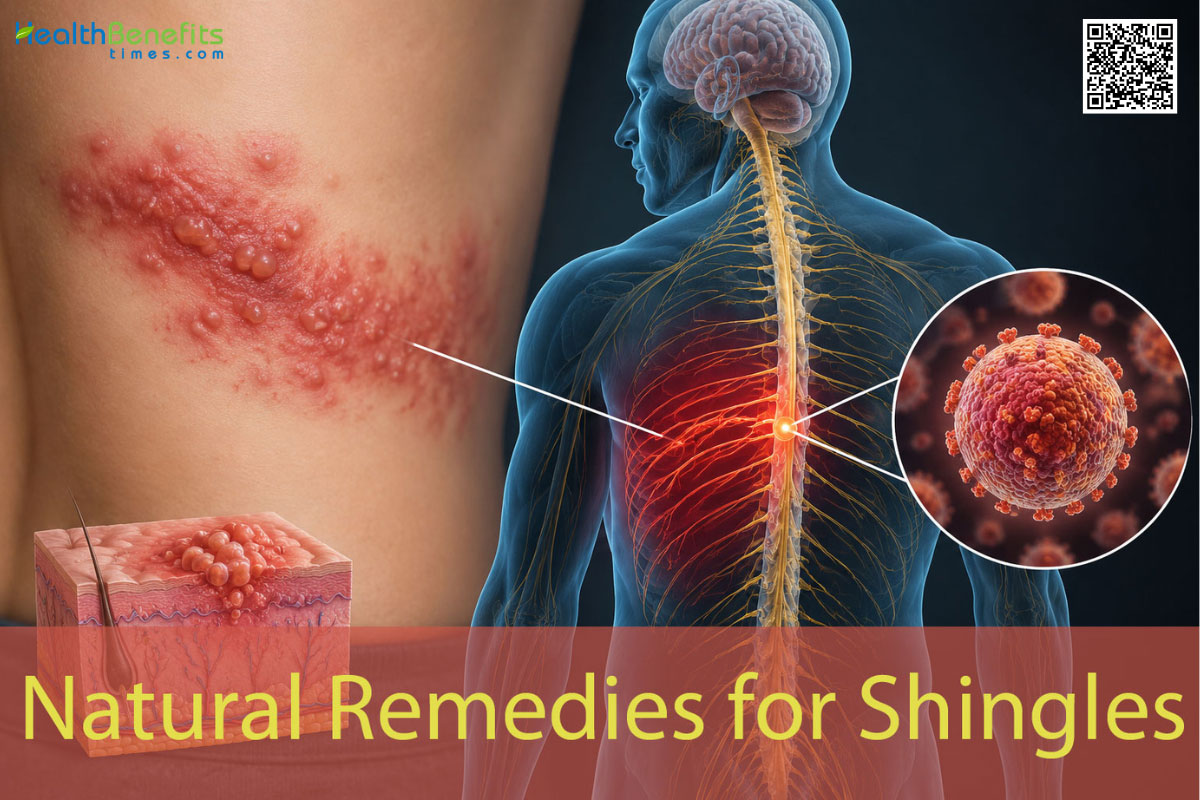
 An unexpected patch of tingling skin that slowly evolves into a painful, blistering rash is the classic hallmark of shingles, medically known as herpes zoster. This uncomfortable illness originates from the varicella-zoster virus, which is the exact same pathogen responsible for causing chickenpox in childhood. After a person recovers from chickenpox, the virus does not leave the body; instead, it retreats into the nervous system and lies dormant within the nerve tissue near the spinal cord and brain. Years or even decades later, the virus can suddenly awaken and travel back along the nerve pathways to the skin. Public health statistics reveal that an estimated one million individuals develop this condition each year in the United States alone. 1 While the condition itself is generally not life-threatening, the intense nerve pain it generates can be highly disruptive to daily life. A defining characteristic of the disease is that the rash usually appears as a single stripe or band of blisters wrapping around either the left or the right side of the torso. 2
An unexpected patch of tingling skin that slowly evolves into a painful, blistering rash is the classic hallmark of shingles, medically known as herpes zoster. This uncomfortable illness originates from the varicella-zoster virus, which is the exact same pathogen responsible for causing chickenpox in childhood. After a person recovers from chickenpox, the virus does not leave the body; instead, it retreats into the nervous system and lies dormant within the nerve tissue near the spinal cord and brain. Years or even decades later, the virus can suddenly awaken and travel back along the nerve pathways to the skin. Public health statistics reveal that an estimated one million individuals develop this condition each year in the United States alone. 1 While the condition itself is generally not life-threatening, the intense nerve pain it generates can be highly disruptive to daily life. A defining characteristic of the disease is that the rash usually appears as a single stripe or band of blisters wrapping around either the left or the right side of the torso. 2
Causes of Shingles
Unlocking the mystery of why this virus suddenly returns requires looking at the factors that compromise the body’s natural defense systems. Several distinct triggers can prompt the sleeping virus to reactivate.
1. Reactivation of the Varicella-Zoster Virus
The fundamental cause of the disease is always the awakening of the chickenpox virus that has been hiding in the body’s dorsal root ganglia. Without a prior chickenpox infection, it is biologically impossible for a person to develop shingles. 3
2. Age-Related Immune Decline
Growing older naturally alters how well the human body fights off pathogens. As people cross the age of 50, their immune systems gradually become less vigilant, making it increasingly difficult to keep the dormant virus suppressed. 4
3. Immuno-compromising Health Conditions
Systemic diseases that attack or heavily burden the immune system create the perfect environment for a viral flare-up. Individuals living with HIV/AIDS, specific cancers like leukemia or lymphoma, or chronic kidney disease face a significantly elevated risk of viral reactivation. 5
4. Psychological and Physical Stress
Emotional turmoil and physical exhaustion can take a very real toll on physical health. Prolonged periods of intense stress, severe fatigue, or even fighting off a secondary illness like a common cold can temporarily drop the body’s immune barriers enough to let the virus escape. 6
5. Immunosuppressive Medical Treatments
Modern medical therapies designed to save lives can sometimes inadvertently open the door to this illness. Patients undergoing radiation or chemotherapy, as well as those taking long-term corticosteroids or anti-rejection drugs for organ transplants, are highly susceptible because their immune responses are artificially lowered. 2
Symptoms of Shingles
Catching the signs of an outbreak early can dramatically improve a patient’s recovery experience. The condition generally unfolds in a predictable sequence of distinct symptoms.
1. Early Nerve Pain and Sensitivity
Long before any visual changes occur on the skin, the affected nerve begins to misfire. Patients frequently report an intense burning sensation, deep aching, tingling, or extreme sensitivity where even the brush of a soft shirt feels agonizing. 7
2. A Distinctive Unilateral Rash
Following the initial pain, a red and inflamed rash erupts on the skin. This rash is famous for its unilateral nature, meaning it almost exclusively affects only one side of the body most commonly the torso, but occasionally the neck or face and rarely crosses the body’s midline. {% my.clevelandclinic.org/health/diseases/11036-shingles %}
3. Fluid-Filled Blister Clusters
The red rash quickly evolves into tight clusters of vesicles, which are small blisters filled with clear fluid. Over the course of a few weeks, these painful blisters will naturally break open, weep fluid, and eventually dry out to form crusty scabs. 2
4. Systemic Flu-Like Discomfort
Fighting a reactivated virus takes a toll on the entire body. It is quite common for individuals to experience a low-grade fever, sudden chills, persistent headaches, stomach upset, and an overwhelming feeling of general fatigue during the acute phase of the outbreak. 5
5. Post-herpetic Neuralgia
Sometimes the pain outlasts the visible illness. A frequent and severe complication of the disease is post-herpetic neuralgia, a condition where the nerve fibers remain damaged and continue to send severe pain signals to the brain long after the skin blisters have completely healed. 4
Shingles Facts
| Category | Details |
| Symptoms |
|
| Causes |
|
| Types of Shingles |
|
| How does spread |
|
| Age Group |
|
| You might be at a higher risk for exposure of this disease if you: |
|
| How doctors diagnose |
|
| Other facts |
|
Natural Remedies of Shingles
1. Healing Baths with Colloidal Oatmeal
Immersing yourself in water can provide immediate relief for inflamed, itchy skin, provided you keep the temperature carefully controlled. You should always run a lukewarm or cool bath, as hot water pulls blood to the surface of the skin and will actively worsen your blister pain. You can add one to two cups of finely milled colloidal oatmeal directly under the running water to maximize the therapeutic effect. The natural anti-inflammatory properties of oats help to repair your broken skin barrier and aggressively reduce the urge to scratch. 8 Note: It is commonly used by soaking the entire body in the oat-infused bath for 15 to 20 minutes daily, followed by gently patting the skin dry with a clean towel to avoid any friction.
2. Soothing Cool Compresses
Altering the temperature of your skin is a highly effective way to trick your nerve endings and dampen sharp pain signals. You can apply a clean, cool, moist cloth directly over the rash to instantly soothe the burning sensation. The gentle coolness naturally constricts the tiny blood vessels just beneath the surface, which pulls away tissue swelling and numbs the area. You must be careful never to use harsh, frozen ice packs directly on your blisters, as extreme cold can actually increase skin sensitivity and trigger deeper nerve pain. 9 Note: It is commonly applied by dampening a soft cotton washcloth with cool water, wringing out the excess liquid, and letting it rest gently over the affected area for 10 to 15 minutes at a time.
3. Baking Soda and Cornstarch Pastes
Encouraging your weeping blisters to dry out and scab over is a crucial milestone in your recovery timeline. You can effortlessly create an absorbent paste using basic pantry staples like cornstarch or baking soda. Both of these fine powders possess excellent moisture-wicking properties that help pull excess fluid out of open sores. Furthermore, baking soda actively alkalizes the surface of your skin, which neutralizes irritating acids and dramatically calms persistent itchiness. 10 Note: It is commonly applied by mixing two parts dry powder with one part clean water to form a thick, spreadable paste, lightly coating the rash, and rinsing it away gently after 15 minutes.
4. Calamine Lotion
Reaching for the classic pink bottle of calamine lotion is one of the most reliable ways to protect a viral skin eruption. You can use this soothing liquid to cool your skin upon contact and calm irritated nerve endings. The primary active ingredient is zinc oxide, which works as a gentle astringent to pull fluid out of the blisters so they can form protective crusts much faster. It also leaves behind a physical chalky barrier that shields your delicate, healing skin from friction and environmental dust. 9 Note: It is commonly applied by dabbing a thin, even layer over the blisters with a sterile cotton ball after a cool shower, allowing it to air-dry completely before dressing.
5. Topical Capsaicin
Harnessing the very compounds that give chili peppers their fiery heat can surprisingly shut down chronic nerve pain. You can find over-the-counter creams containing capsaicin, a natural botanical extract, to manage the deep aches associated with your rash. Capsaicin provides relief by safely depleting a specific chemical messenger in your body called “Substance P,” which is directly responsible for carrying pain signals from your raw nerve endings to your brain. 11 Note: It is commonly applied as a commercial cream, rubbed very lightly into the affected area three to four times a day, but only after the blisters have fully closed and crusted over.
6. Medical-Grade Manuka Honey
Bees manufacture some of the most potent natural medicine available, and certain specialized honeys are phenomenal for cellular skin repair. You can apply medical-grade Manuka honey to your rash to take advantage of its rich antibacterial and anti-inflammatory properties. Fascinating laboratory research has shown that specific honeys even possess direct antiviral activity against the varicella-zoster virus. 12 The natural sugars in the honey also create an osmotic gradient, gently drawing moisture and protective healing nutrients into the damaged tissues. Note: It is commonly applied by spreading a very thin, even layer of the honey directly over the rash and covering it lightly with a non-stick sterile gauze bandage to protect clothing.
7. Witch Hazel Extract
Distilled from the leaves and bark of a native North American shrub, this clear liquid acts as a gentle powerhouse for skin recovery. You can use pure witch hazel on your rash to benefit from its incredibly high tannin content. These natural plant compounds act as powerful astringents that shrink swollen, inflamed tissues and help stop the weeping of open blisters. Recent scientific evaluations have demonstrated that witch hazel actively decreases pro-inflammatory markers in the skin, facilitating a much calmer healing environment. 13 Note: It is commonly applied by saturating a sterile cotton pad in the liquid and gently pressing or dabbing it onto clean, dry skin without rubbing or scrubbing.
8. Dietary L-Lysine
Adjusting what you put on your plate can directly influence how the virus behaves internally. You can focus on eating foods that are naturally rich in L-lysine, which is an essential amino acid. Inside the human body, viruses rely heavily on a different amino acid called arginine to replicate and build their viral structures. Because lysine naturally competes with and suppresses your body’s absorption of arginine, boosting your lysine intake may help stall the virus’s ability to multiply, supporting a much faster overall recovery. 14 Note: It is commonly eaten by incorporating high-lysine whole foods into your daily meals, such as plain yogurt, cheese, wild-caught fish, poultry, and lean meats.
9. Vitamin B12 and B-Complex
Repairing the microscopic damage done to your nerve fibers requires the right nutritional building blocks. You can support your nervous system’s recovery by ensuring adequate intake of Vitamin B12 and a full spectrum B-complex supplement. Vitamin B12 is uniquely responsible for protecting and calming the nervous system, while aiding in the regeneration of the myelin sheath that insulates your nerves. Ensuring your body has ample B vitamins can potentially reduce the severity of the tingling and burning sensations. 15 Note: It is commonly used as an oral sublingual drop, a daily dietary capsule, or through dietary sources like eggs and nutritional yeast to actively support nerve tissue repair.
10. Turmeric, Ginger, and Garlic
Your kitchen spice rack contains potent, scientifically backed compounds that support immune function and dull systemic pain. You can rely on turmeric, ginger, and garlic to act as natural, dietary anti-inflammatories. Turmeric contains an active compound called curcumin, which naturally blocks the exact same pain-causing enzymes in the body that many over-the-counter painkillers target. 16 Garlic offers robust antimicrobial benefits, while ginger acts to calm systemic inflammation and soothe any nausea or stomach upset that accompanies the viral attack. Note: It is commonly eaten by crushing raw garlic into savory meals, brewing fresh ginger root into warm teas, or blending turmeric with a pinch of black pepper and coconut oil to make a comforting beverage.
11. Essential Oils (Oregano, Lemon Balm, and Wintergreen)
Aromatic plant extracts carry concentrated defensive compounds that can assist in managing viral symptoms. You can explore the use of essential oils like oregano, lemon balm, and wintergreen to calm the skin. Oregano oil is highly regarded for its aggressive antiviral properties, while lemon balm is frequently included in skin preparations for its soothing, anti-inflammatory nature. Wintergreen contains natural salicylates, closely related to aspirin, which provide a mild numbing effect when applied to aching areas. 10 Note: It is commonly applied topically only after being heavily diluted—usually a few drops mixed into a tablespoon of a plain carrier oil like coconut or olive oil—and gently massaged around the borders of the rash.
12. Echinacea and St. John’s Wort
Herbal medicine offers specific plants targeted at boosting white blood cells and easing nervous tension. You can utilize Echinacea, a purple coneflower historically used to strengthen the immune system’s response to viral invaders by stimulating white blood cell production. Additionally, St. John’s Wort has a long history in traditional medicine for supporting nerve pain and easing the mild anxiety or depression that often accompanies long-term, painful conditions. 17 Note: It is commonly used by brewing the dried herbs into a warm, comforting tea or taking them in standardized tincture or capsule forms as directed by a healthcare professional.
13. Acupuncture Therapy
Ancient practices involving energy pathways are finding solid footing in modern pain management. You can seek out a licensed acupuncturist to help manage both the acute pain of your outbreak and any lingering postherpetic neuralgia. By inserting incredibly fine needles into specific points on the body, acupuncture helps stimulate the central nervous system to release natural, pain-killing endorphins. Recent clinical reviews indicate that acupuncture shows moderate to significant benefits in pain relief and sleep improvement for patients struggling with nerve damage. 18 Note: It is commonly applied during a 30-to-60-minute clinical session where a practitioner places needles in strategic areas away from the active rash to trigger systemic pain relief.
14. Red Light and Cold Laser Therapy
Modern phototherapy uses specific wavelengths of light to encourage cellular repair without generating heat. You can explore red light or cold laser therapy as a non-invasive way to decrease inflammation deep within the nerve tissues. This therapy works by stimulating the mitochondria within your cells, essentially giving them more energy to repair the damage caused by the virus. Many patients report a noticeable reduction in the sharp, branding-iron pains and tissue swelling after several sessions. 19 Note: It is commonly used by exposing the affected area to a specialized clinical light device for brief, 10-to-20-minute sessions several times a week.
15. Yoga and Mindful Meditation
Emotional distress and chronic pain are deeply intertwined, and movement therapies are excellent tools for breaking that cycle. You can practice gentle yoga postures and mindful breathing techniques to actively lower your body’s stress response. Severe pain triggers a state of hyper-arousal in your nervous system, but engaging in deep, rhythmic breathing forces the body into a “relaxation response.” Research demonstrates that mindful practices effectively reduce overall pain intensity, lower stress hormones like cortisol, and significantly improve sleep quality. 20 Note: It is commonly used by engaging in 15 to 20 minutes of guided deep breathing, quiet meditation, or extremely gentle, non-strenuous stretching exercises daily in a comfortable space.
Foods and Activities to Avoid When You Suffer from Shingles
While you are actively nurturing your body, you must also be vigilant about removing obstacles to your healing. You should be mindful to steer clear of specific dietary triggers and physical habits that fan the flames of inflammation or encourage the virus to linger.
1. Arginine-Rich Foods
Because the virus actively utilizes the amino acid arginine to help build its viral structures, you should temporarily cut back on foods that contain high concentrations of it. You will want to avoid snacking on chocolate, peanuts, almonds, walnuts, sesame seeds, and gelatin-based products until your outbreak has fully resolved. 21
2. High-Glycemic and Sugary Foods
Feeding your body empty calories makes it harder for your immune system to do its job. You should avoid candies, baked goods, sugary breakfast cereals, and sweet beverages. Rapid spikes in your blood sugar trigger the release of inflammatory molecules and free radicals, which place unnecessary stress on your body and distract your immune defenses. 22
3. Highly Processed Foods and Saturated Fats
Convenience foods often come with a hidden cost to your cellular health. You should steer clear of pre-packaged snacks, deep-fried items, and fatty meats that are heavy in saturated fats and excess omega-6 fatty acids. These ingredients trigger widespread systemic inflammation, which can drastically slow the healing of your damaged nervous system.
4. Alcohol Consumption
Numbing the pain with a drink is highly counterproductive to your recovery. It is strongly recommended that you avoid alcohol completely during an active outbreak. Alcohol aggressively suppresses your immune system, dehydrates your tissues, and can interact dangerously with prescription pain relievers or antiviral medications you might be taking. 23
5. Swimming in Public Pools
Taking a dip in the pool is one of the worst things you can do for an active rash. You must never go swimming in public waters while you have unhealed blisters. Not only can the fluid from your rash spread the chickenpox virus to vulnerable people in the pool, but the chlorine does not kill the virus, and the chemicals will severely irritate your open sores. 24
6. Strenuous Exercise and Heavy Sweating
Pushing your physical limits while sick will only exhaust your reserves. While gentle movement like walking is perfectly fine, you should avoid heavy cardiovascular workouts or intense weightlifting. Excessive sweating and physical friction from tight workout clothes will irritate the rash and can easily introduce bacteria into open blisters, causing dangerous secondary skin infections. 25
Myths and Misconceptions
Rumors and outdated information about this illness circulate frequently, leading many people to misunderstand their risks and available treatment options. Clearing up these common fallacies is vital for proper awareness and care.
1. Only the Elderly Can Contract It
While it is an undeniable fact that the risk jumps significantly after the age of 50 due to a natural decline in immune function, anyone who has previously had chickenpox remains susceptible. Healthy young adults, teenagers, and even small children can and do experience outbreaks if their immune systems undergo a period of intense stress or illness. 26
2. It is Exactly the Same Illness as Chickenpox
Although both conditions are triggered by the exact same pathogen (the varicella-zoster virus), the diseases manifest in entirely different ways. Chickenpox is usually a mild, highly contagious, full-body childhood illness, whereas shingles is a localized, highly painful nerve reactivation that primarily strikes adults and requires different management. 27
3. It is Not Contagious at All
You cannot give another person this specific disease directly, but the fluid inside the rash blisters is indeed highly contagious. If a person who has never had chickenpox or the varicella vaccine touches that fluid, they can contract the virus and will develop a primary chickenpox infection as a result. 28
4. The Visible Skin Rash is the Only Problem
The blistering rash is certainly the most visual and recognizable sign, but it is rarely the most troubling aspect of the disease. The underlying nerve damage often causes severe pain that begins days before the rash ever appears and, in unfortunate cases, can persist for months or years after the skin has completely healed. 29
5. You Can Only Get It Once in Your Lifetime
A vast majority of individuals will thankfully only experience one episode, but there is absolutely no guarantee of lifelong immunity after an outbreak. It is entirely possible for the virus to reactivate a second or even a third time if the immune system becomes sufficiently compromised later in life. 1
Special Considerations
The severity, management, and long-term outlook of this illness can look remarkably different depending on a person’s age, life stage, and underlying medical background.
1. Children
Spotting a blistering nerve rash on a young child can be incredibly alarming for parents, but pediatric cases are generally quite rare. When the condition does occur in children, the symptoms tend to be much milder than the excruciating pain typically seen in adults. A child is mostly at risk if they experienced a primary chickenpox infection before they were one year old, or if their immune system is currently suppressed by conditions like pediatric cancer or specific medical treatments. 34
2. Pregnancy
Expectant mothers facing an outbreak understandably worry about the health of their unborn child. Fortunately, developing this specific viral rash during pregnancy rarely causes severe complications or birth defects for the baby. The main medical concern lies in managing the mother’s pain safely without harmful drugs and ensuring she does not pass the virus to her newborn if the rash is still active and weeping during delivery. 31
3. Chronic Conditions
Living with pre-existing health issues vastly complicates the recovery timeline. Individuals with chronic cardiovascular disease, diabetes, or autoimmune disorders like rheumatoid arthritis face up to a 27% higher risk of experiencing a viral reactivation. 32 Furthermore, the aggressive inflammation generated by the virus puts temporary, heavy stress on the heart, highlighting the need for careful medical management in patients with an established cardiovascular history.
4. Elderly
The aging body faces the steepest uphill battle against this virus. Adults over the age of 60 not only represent the largest demographic of patients, but they also bear the absolute highest risk for severe, lasting complications. Older adults are significantly more susceptible to developing postherpetic neuralgia, a condition where the nerve pain becomes a chronic, debilitating fixture that severely impacts sleep, mobility, and overall quality of life. 5
Precaution Before Use of Natural Remedies When You Have Shingles
While holistic approaches offer wonderful support, natural ingredients are powerful and must be respected. You should always exercise a high degree of caution before applying anything new to an angry, active rash.
1. Consult Your Healthcare Provider First
You should never use natural remedies as a strict replacement for a professional medical evaluation. Always inform your doctor about any herbs, supplements, or sudden dietary changes you wish to try, as some natural compounds can interact poorly with prescription antiviral medications or painkillers.
2. Never Apply Raw Essential Oils Directly
Essential oils are incredibly potent, highly concentrated plant extracts. You must always dilute them properly in a gentle carrier oil—such as coconut, almond, or olive oil—before placing them anywhere near your skin to prevent chemical burns and severe contact dermatitis. 10
3. Avoid Using Thick Creams on Weeping Blisters
You should reserve thick lotions, heavy cosmetic creams, and capsaicin ointments solely for skin that is intact or fully crusted over. Applying heavy, occlusive creams to open, oozing sores traps bacteria against the wound bed and prevents the blisters from drying out naturally.
4. Always Perform a Skin Patch Test
Your immune system is already on high alert and highly reactive during a viral outbreak. Before covering a large area of your rash with a new topical remedy, you should test a tiny amount on an unaffected piece of skin to ensure you do not trigger an unexpected allergic reaction.
5. Monitor Closely for Signs of Bacterial Infection
You must watch the visual progression of your rash closely. If a natural remedy causes increased redness, spreading swelling, heat, or a sudden spike in throbbing pain, you should wash it off immediately with mild soap and water, as it may be irritating the skin barrier or masking a secondary bacterial superinfection.
When to See a Doctor
Self-care and natural soothing techniques are fantastic supplementary tools, but certain red-flag situations demand immediate professional medical intervention to prevent permanent bodily harm.
1. The Rash Appears Near Your Eye or Face
You must seek emergency medical care the moment you notice blisters developing anywhere on your forehead, nose, or near your eyes. Known medically as herpes zoster ophthalmicus, this specific presentation can rapidly lead to permanent vision loss, corneal scarring, or severe eye damage if left untreated. 33
2. You Are Over the Age of 60
Because age is the single biggest risk factor for long-term complications, you should not try to wait out the virus alone. You should consult a doctor promptly to receive prescription antiviral medications, which are most effective when taken within the first 72 hours of the rash appearing to halt viral replication. 7
3. You Have a Weakened Immune System
If you are living with cancer, HIV, or take immunosuppressive drugs for any reason, you should contact a physician immediately. Without a strong immune defense to wall off the infection, the virus can spread rapidly and dangerously to internal organs, brain tissue, or the spinal cord. 2
4. The Pain Becomes Utterly Unmanageable
If over-the-counter pain relievers, cool baths, and holistic remedies fail to take the edge off your suffering, you should speak to a healthcare provider. They can prescribe specialized nerve-blocking agents, anticonvulsants, or topical anesthetic patches to help you cope with extreme discomfort.
5. The Rash Becomes Widespread
You should get medical help immediately if the blisters do not remain confined to a single, localized stripe. If the rash begins aggressively spreading across multiple dermatomes or appearing on both sides of your body, it indicates a much more severe, disseminated infection that requires aggressive clinical care.

